What Are Blood Components?
Blood Components
Today, when you walk into a Modern Blood Bank asking for blood, you are very likely to be asked “Which Component?” Days are gone when only Whole blood was the prescribed transfusion practice. Nowadays, blood is separated into various types of blood components using the technique of centrifugation. At our highly modernised Component separation laboratory in the Blood Bank all the collected whole blood units are separated into different components to meet the patient requirements.
Packed Red Cells (PRC)
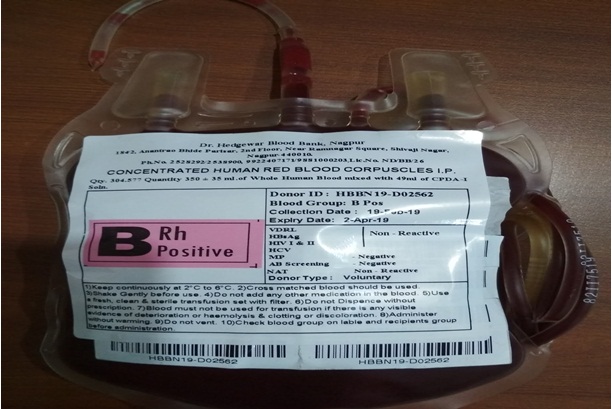
- It also called as PRBC (Packed Red Blood Cells).
- Each red blood cell has haemoglobin that carries oxygen to the cells of the body and transports carbon dioxide from the cells to the lungs for excretion.
- Manufactured in the bone marrow, red blood cells are continuously being produced and broken down.
- They live for approximately 120 days in the circulatory system before they are removed by the spleen.
- Indicated in patients with anaemia or bleeding secondary to trauma, surgery or childbirth.
- The shelf life of Packed Red Cells is 35 days without additive solution and 42 days with additive solution.
Random Donor Platelet Concentrate (RDP)
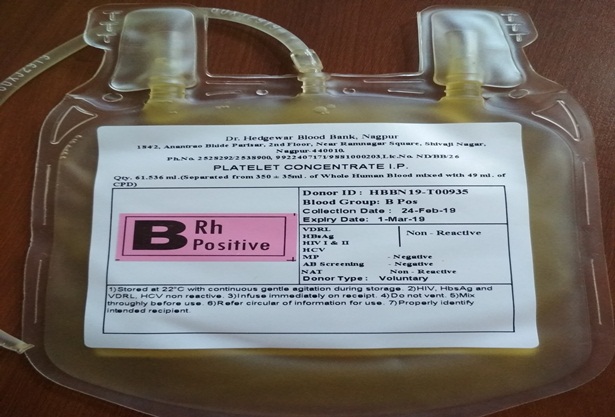
- It also called as PC (Platelet Concentrate).
- These are small cell fragments in your blood whose main function, along with clotting factors, is to stop bleeding.
- When a blood vessel is damaged, platelets will become “glued” together at the damage site to form a platelet plug, which prevents blood from leaking out.
- Indicated in patients with bleeding, patients undergoing surgical procedures, patients with blood cancers, dengue patients and cancer patients on chemotherapy.
- The shelf life of Random Donor Platelet Concentrate is 5 days.
Fresh Frozen Plasma (FFP)
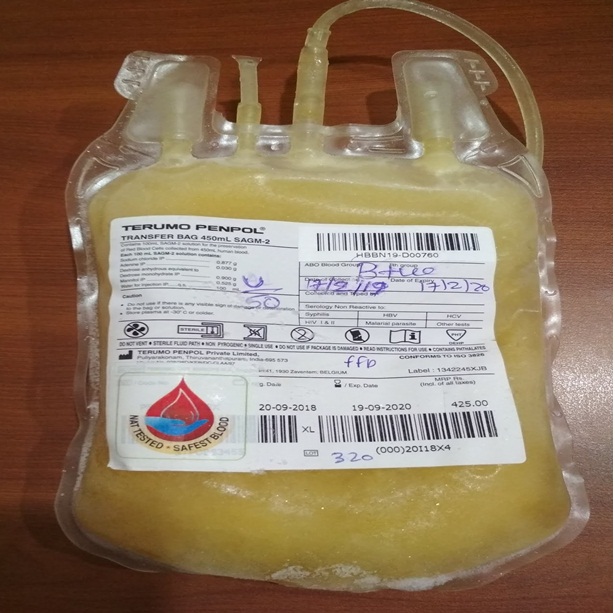
- Plasma is frozen soon after separation to maintain the activity of blood-clotting factors.
- It can be stored for up to 12 months at – 40°C or below.
- Single-donor packs which must be thawed before use, usually in a purpose-designed waterbath.
- FFP is indicated for the treatment of patients with bleeding due to multiple clotting factor deficiencies, disseminated intravascular coagulopathy, Liver disease, Dilutional coagulopathy in massive transfusion, Correction of bleeding due to excess warfarin.
- The shelf life of Fresh frozen Plasma is 1 year.
Single Donor Platelet Concentrate (SDP)
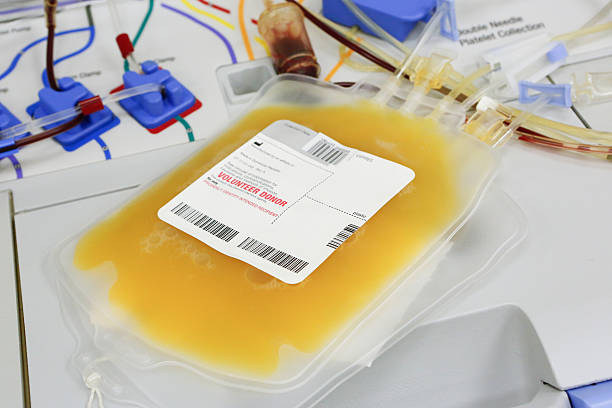
- Apheresis platelets are usually called 'Single Donor Platelets' because they are collected from a single donor with an automated cell separator.
- Platelet apheresis is a medical procedure of removal of platelets that involves directing the donor’s blood through tubing to a machine which separates blood components. Blood is withdrawn through a needle and mixed with an anticoagulant (citrate) to prevent clotting. The separation of blood components is done by a centrifugation process in the machine. Platelets are removed, while the remainder of the blood components are reinfused back into the donor. All the tubing and needles used in this process are sterile and disposable.
- A single donor platelet concentrate contains a minimum of 3.0 X 1011platelets suspended in approximately 200 mL of plasma, which is the equivalent of 6 to 8 random donor platelet concentrates. The shelf life of Single Donor Platelet Concentrate is 5 days.
Leukoreduced Packed Red Cells (LRPRC)

- Leukocytes (White Blood cells) are present in donated blood, they serve no purpose, but are transfused along with red blood cells, platelets or plasma. Leukocytes may carry viruses that cause immune suppression and release toxic substances. Studies have shown that removing leukocytes from donated blood may have a number of benefits for patients.
- Leuko-reduction is the removal of white blood cells (or leukocytes) from the blood or blood components supplied for blood transfusion. After the removal of the leukocytes, the blood product is said to be leukoreduced.
- It is unit of blood from which more than 70% of Leucocytes are removed.
- Benefits of Leukoreduction
1. Reducing the frequency and severity of Febrile Non-Hemolytic Transfusion Reactions (FNHTRs).
2. Reducing the risk of cytomegalovirus (CMV) transmission.
3. Reducing the risk of HLA-alloimmunization and platelet-refractoriness.